Delaying immunisation against COVID-19 in children is an important step in offering a more suitable vaccine, argues Dr Hamid Merchant.
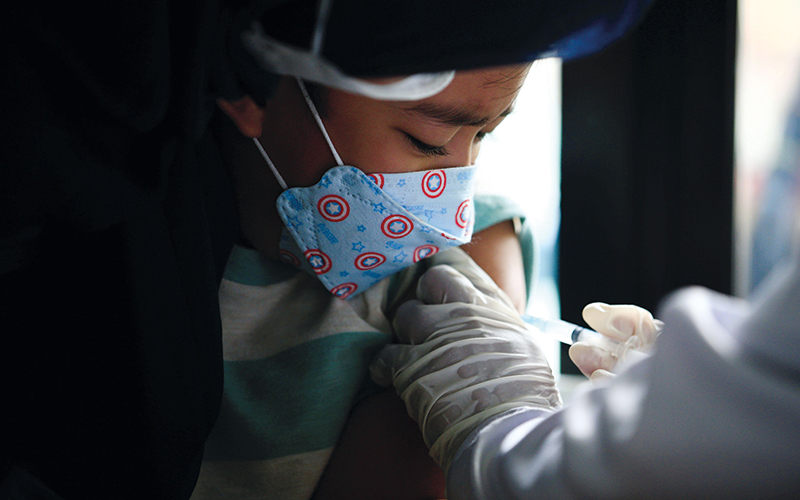
In February 2022 the government’s Joint Committee on Vaccination and Immunisation (JCVI) advised that COVID-19 vaccines in 5- to 11-year-old children not in a clinical risk group are not essential, and shouldn’t displace the delivery of other paediatric immunisation programmes. Some non-COVID-19 paediatric vaccination programmes had fallen behind as a result of the pandemic, resulting in health inequalities.
The statement drew criticism from some in the healthcare community who argued that a mandatory mass immunisation programme against the virus is necessary for children. “As a pharmaceutical scientist with extensive experience in pharmaceutical product development, like many, I had been following COVID-19 therapeutics and vaccines very closely,” says Dr Hamid Merchant, Subject Leader in Pharmacy at the University of Huddersfield. “I decided to write an article in response to the controversy as to why COVID-19 vaccines for young children hadn’t been approved in the UK but had in the US, and why the UK was so slow to respond.”
In Why COVID vaccines for young children are not essential at this moment in time?, Merchant suggests that a public health policy should not “rush mass-immunising young children”. He argues that delayed immunisation can be beneficial in offering a more suitable formulation for children, such as the nasal COVID vaccine that will provide protection against infection and transmission.
Vaccine differences
During the initial phase of rollout, most healthcare professionals feared that discussing openly the necessity of the vaccine in special populations such as children would undermine vaccine uptake, Merchant says. This meant open dialogue and personalised vaccine recommendations, such as taking into consideration each patient’s medical history, comorbidities, current and past medication history, were avoided.
“The later acknowledgement of COVID vaccine-induced thrombotic thrombocytopenia, Guillain–Barré Syndrome and myocarditis/pericarditis by the Medicines and Healthcare products Regulatory Agency, European Medicines Agency and the Food and Drug Administration [in the US] was a major step change among the public health community,” Merchant says.
“It encouraged open discussions about potential rare side effects and the need for individualising risks and benefits for special populations, including children.”
Merchant says that it’s time the scientific community discusses the vaccine science and differences between various formulations that have been approved by the regulatory agencies.
“We shouldn’t rush for a one-size-fits-all approach, particularly when there is a product out there which would be of greater benefit to children,” he adds.
Vaccine efficacy
In the paper, Merchant points out that current COVID-19 vaccines were designed using the variant of the virus that was prevalent in early 2020, and since then the virus has significantly mutated. While they may still provide protection against severe COVID-19, risk of hospitalisation and admission to intensive care, and death – all rarely seen in children – they will not provide children with protection from catching the virus in the first instance. Nor will they prevent minor illness or reduce the risk of the virus spreading around the community.
“Moreover, JCVI noted that over 85% of children aged 5–11 years contracted COVID-19 in January 2022 during the Omicron outbreak in UK and, therefore, have already acquired natural immunity that will still provide protection in healthy children against severe disease on future reinfection,” he adds.
As current vaccines are injected intramuscularly, they cannot protect against catching the respiratory virus in the first place, nor do they produce the mucosal antibodies that provide the protection at the point of entry for the virus, Merchant explains. “This is normally the case with all respiratory pathogens and corresponding injectable vaccines, for instance, flu,” he writes. “Injectable flu vaccines, therefore, were not very successful historically in offering the level of protection sought from the mass children immunisation campaign.”
The nasal flu spray – given to school-going 2 to 17 year olds in England – does, however, prevent children catching the infection in the first place and blocks community transmission, Merchant explains. “The annual flu immunisation campaign was a great example that every healthcare professional can easily relate to, so I tried in this article to highlight the significant benefits that we have seen by moving away from conventional injectable flu jabs to modern nasal vaccines for mass immunisation in children,” he adds.
Another consideration is the significant variation in children aged 5 to 11 years of deltoid muscle mass, meaning it’s not easy to standardise the dose and administration technique of the vaccine. For this reason very young children with minimal deltoid mass are often contraindicated for intramuscular injections in the arm.
Next-generation vaccines
As someone who started his career in investigational pharmaceutics in one of the biggest pharmaceutical companies, Merchant is trained in establishing pharmaceutical causes of mysterious adverse drug reactions, to better formulate products. He has also developed expertise in clinical pharmaceutics, understanding the biological interactions of pharmaceutical formulations and their components, and their effects on product efficacy and safety.
“Not all products are made the same and can therefore not behave exactly the same; there may always be a better choice for a particular patient,” he says. “Pharmacists are a key player in the healthcare system and should always be a fundamental part of the healthcare team.”
He believes the paper has made a significant difference in explaining the science behind vaccine formulations and how not all formulated vaccine products behave or work the same way, albeit made for same purpose. “If we had a choice, a formulation may well be more suitable for an individual than others,” he adds.
“I think it has made an important contribution to initiate a thought process among healthcare professionals and did manage to start a scientific dialogue and discussion among scientists and public health professionals across the world in revaluating their position on child vaccine mandates within their communities. We still need to do more in disseminating this information to public health authorities and policymakers around the world.”
As the vaccines have done their job of enabling COVID-19 to become endemic, it’s imperative to continue investigating the next generation of COVID vaccines for all those who remain at high risk from emerging variants of concern, Merchant concludes.

- Subject Leader in Pharmacy at the University of Huddersfield
- Adjunct Professor at the Health Services Academy, Government of Pakistan
- Extensive experience working for and with pharmaceutical industries
- Completed PhD in pharmaceutics, University College London
- Received a Bachelors and a Masters in Pharmacy from University of Karachi, Pakistan.
Image credit | Reuters_Alamy | iStock