Lecturer in Molecular Microbiology Tina Joshi looks at the detection of antimicrobial-resistant bacteria in the timeframe of a doctor’s appointment.

By 2050, it is estimated that 10 million people worldwide will die per year as a result of being infected with antimicrobial-resistant (AMR) bacteria, costing approximately $100 trillion in lost output. The roots of antibiotic resistance lie within the genetic make-up of the bacteria themselves, which evolve to survive antibiotic action and persist. This process appears to have been accelerated by the inappropriate use of antibiotics within healthcare, coupled with the lack of new antibiotics in the discovery pipeline and lack of suitable and accurate diagnostics in development. This impending AMR crisis has led researchers and governments to accelerate diagnostics and drug development globally.

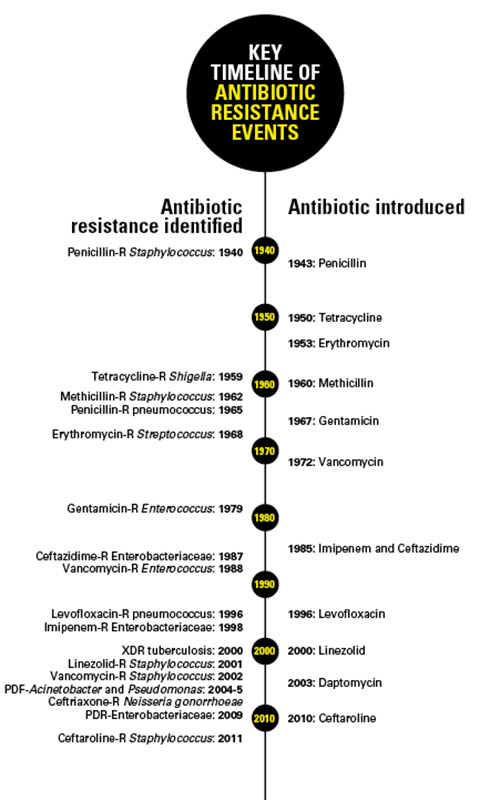
Worryingly, the last discovery of a major new class of antibiotics was over 30 years ago and the majority of bacterial diagnostic technologies have yet to advance from 70 years prior without use of the gold standard of microbial culture. Interestingly, the development of new affordable, accurate, fast and simple tests for bacterial infections is the focus of the Longitude Prize announced by NESTA in 2014, and voted for by the public as the challenge of our time. The prize aims to encourage the global development of diagnostics, which will enable health professionals to administer the appropriate antibiotic in a timely fashion.
Five minutes
This is also the focus of the research group that I lead at the University of Plymouth, where we are developing a diagnostic device that is able to specifically detect AMR genes from pathogens at point-of-care within the timeframe of a doctor’s appointment – that is within five minutes – in line with the recommendations made by the report into AMR by Lord Jim O’Neill, published in 2016.
The technology aims to reduce the inappropriate prescribing of antibiotics in the GP surgery and to detect antibiotic-resistant infections rapidly. Indeed, in 2013, a total of 27 million prescriptions for antibiotics were given to patients in the UK when only 13 million were needed; and this doesn’t take into account the ease with which antibiotics can be purchased over the counter in certain countries and their use in agriculture globally.
The diagnostic technology utilises two components – a rapid microwave DNA extraction methodology, and aptamer-based sandwich assay; both of which were designed in my previous post-doctoral posts at Cardiff University. These post-doctoral posts were focused on the development of real-time point-of-care detection assays for the bioterrorism agent Bacillus anthracis, methicillin-resistant Staphylococcus aureus and the nosocomial pathogen Clostridium difficile, for which patents have been filed. The uniqueness of the assay in development is the rapid lysis of bacteria using precision microwaves within five seconds to release DNA directly from a sample without any prior purification, combined with a highly specific five minute lab-on-a-chip assay targeted to the genes conferring resistance to certain antibiotics.
What’s the frequency?
Microwaves have been routinely used in medicine for ablation of tumours, imaging and microbial decontamination. Interestingly, conventional microwave ovens have been shown to release DNA from microorganisms via lysis at a frequency of 2.45 GHz. However, the microwaves within conventional microwave ovens are not precisely focused toward the sample and generate heat during the microwaving process. While this is great for heating food, it isn’t great for releasing stable DNA for detection, as DNA is denatured during the heating process. Further, microwave ovens are cumbersome and do not lend themselves to be used at point-of-care. Thus there was a need to develop a microwaving system that could be integrated into a hand-held point-of-care detection device. In collaboration with Cardiff University, I helped design a bench-top microwave lysis system, which is able to deliver high precision, pulsed microwaves to a raw clinical sample. These microwaves lyse the target pathogen and instantaneously release stable DNA for detection.
In my new laboratory at the University of Plymouth, I am building upon this knowledge to develop a new portfolio of hand-held diagnostics for various pathogens and targets based on my lab-on-a-chip chemistry.
The challenges
In the UK, one in four people are infected with the antibiotic resistant urinary tract pathogen E. coli, and thus this is where I’m currently focusing the first iterations of my detection device. Other iterations include diagnosis of AMR pathogens at point-of-care in low/medium economically developing countries and tropical areas, which can make significant life-saving impacts.
Research such as this spans disciplines including chemistry, materials science, communications, microbiology and engineering. The main challenge is to bring everyone together to work on a common goal. Frontier science and new innovations rely on collaborative networks of scientists and each has a share in the tangible generation of a new product from the ideas stage. Beyond this, other challenges are emerging with integration of the device into a hand-held prototype, which can be commercially viable and ensuring that this innovation will not fall into the “Valley of Death”, where so much innovative research unfortunately descends.
I feel lucky to be able to collaborate with such a diverse group of researchers from several disciplines to make a difference. The advent of antibiotic resistance is a global concern and, at present, the technology developed here has real potential to be used at point-of-care and in combatting AMR through providing real-time assistance to clinicians. The scope and impact of this research was recently recognised by the NRI Welfare Society of India, which awarded me with the Hind Rattan 2018 or “Jewel of India” award for non-resident Indians who have made a significant contribution to their country of birth and simultaneously “held the Flag of India high”.
I also regularly discuss this research at public events and am set to be featured in a soon-to-be-announced BBC documentary about how scientists are combatting AMR.
Tina Joshi is a Lecturer in Molecular Microbiology at the University of Plymouth.