Professor Kevin Harrington discusses his recent research into how the herpes simplex virus can be used to destroy cancer cells.
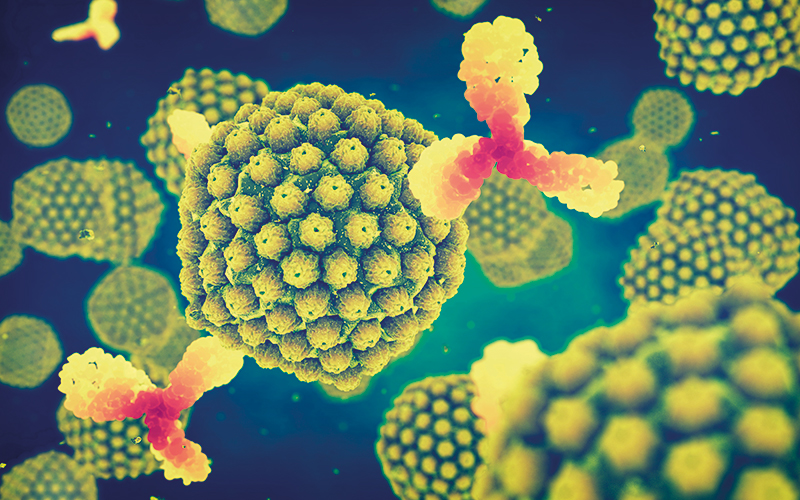
The herpes simplex virus might appear an unlikely biological ally in the fight against cancer, but a small study carried out by a team from the Institute of Cancer Research and The Royal Marsden NHS Foundation Trust suggests that the virus responsible for cold sores may be able to give hope to people whose cancers have previously resisted all other standard attempts at treatment.
Early findings presented at the recent European Society for Medical Oncology Congress in Paris showed that a version of herpes simplex that had been genetically modified to infect and kill cancer cells was effective in a quarter of patients with different types of advanced cancer, such as skin, head and neck and oesophageal.
Called RP2, the modified herpes virus has been tweaked to attack cancer cells on two fronts. After being injected directly into tumours, it first replicates itself inside the cancer cells to the extent that it causes them to burst; it then inhibits a protein called CTLA-4, and by doing so helps to trigger a response in the patient’s immune system, effectively kick-starting the ability to identify and destroy cancer cells.
Shrunken tumours
Around 40 patients were involved in the trial at The Royal Marsden NHS Foundation Trust. Some of those patients received the RP2 virus on its own, others were given it in combination with an immunotherapy drug called nivolumab. Three out of nine patients given just RP2 responded positively with shrunken tumours. Seven out of 30 of those on the combined treatment showed progress.
The lead researcher, Kevin Harrington, Professor of Biological Cancer Therapies at The Institute of Cancer Research, London, and Consultant Clinical Oncologist at The Royal Marsden NHS Foundation Trust, says that the herpes virus has a number of features that make it a good candidate for cancer treatment.
“There’s a strong track record for using these viruses. We can easily modify the behaviour of the viruses and they can infect a wide range of cancer cells. In all, they are a really good choice, and the versions we have been developing are the most refined versions that exist so far.”
The microbiology of the herpes simplex virus is well understood and it is also largely safe, though one of the main objectives of the trial was to see just how safe. “We did see some inflammation and swelling in the lumps and bumps where the virus was injected and some patients did develop fever and a mild flu-like illness,” says Harrington. “But it was very transitory. It tended to start about six hours after the injection and then cleared within 12 to 18 hours. Then as we went through the sequential injections, any side effects tended to become less severe.”
Just kills cancer cells
Another key safety feature the RP2 is that the genetic modification allows it to grow in cancer cells only, so there’s no possibility of it trying to attack healthy cells. “It kills just cancer cells. It bursts them open and in doing so, it raises a red flag to the immune system. In addition, we’ve modified the virus so that it expresses a protein that activates a strong signal to the immune system.”
This is the antibody ipilimumab, which binds to CTLA-4, preventing it from carrying out its normal function of helping to restrain the immune system. “This is neat,” says Harrington, “because it avoids the systemic toxicity of ipilimumab. Normally, this drug can be given intravenously, but expressing it within the tumour via a virus means that patients don’t have to suffer the side effects of it being given to the whole body.”
Harrington describes the outcomes for the three patients treated positively with just RP2 as “really outstanding responses, very heartening”. One of those three patients enjoyed an especially outstanding and heartening result. In May 2017, 39-year-old Krzysztof Wojkowski was diagnosed with a type of salivary gland cancer. After several operations, he was told that he had run out of treatment options. Then, in 2020, he was given the opportunity to join the RP2 trial. “It was my final lifeline,” he reported. “I had injections every two weeks for five weeks, which completely eradicated my cancer. I’ve been cancer-free for two years now, it’s a true miracle, there is no other word to describe it.”
“It kills just cancer cells. It bursts them open and in doing so, it raises a red flag to the immune system”
The other phase of the study, which combined RP2 with the immunotherapy antibody drug nivolumab, also yielded promising results for a number of patients. “Most pleasingly,” says Harrington, “among patients with cancers that are really difficult to treat or with diseases where the treatment with immunotherapy had already failed, we saw substantial and durable responses. For me, that’s the most telling part of this study. We have treated difficult-to-treat diseases, so this could open up a whole new range of options for these patients.”
The cancer-free goal
Larger and more in-depth clinical trials are now needed to test just how effective RP2 might be at treating cancers that have otherwise proved impervious to established therapies. But is it a realistic aim ultimately to eradicate cancer or is the best hope for some patients to control the disease and learn to live with it? “I think with immunotherapy we have a number of patients who achieve durable states of partial remission. There is some disease, but the disease is under control,” says Harrington. “But really the goal of this treatment, and I think of most other treatment, is to render the patient cancer-free. That’s exactly what we are seeking to do, and we have shown that we are able to achieve that. But if we can’t achieve that, then we will settle for a state of stable disease or partial remission that is long-term and durable. And patients can often manage with that, but obviously the goal is still to eradicate all the disease.”
Professor Kevin Harrington

- Studied medicine at St Bartholomew’s Hospital, London
- PhD student at Hammersmith Hospital, where he began focusing on head and neck cancer
- Completed post-doctoral research in molecular medicine at the Mayo Clinic, Minnesota
- Appointed a Consultant Oncologist at The Royal Marsden in 2001
- Appointed Team Leader in targeted therapy at the Institute of Cancer Research in 2001.
Image credit | Science-Photo-Library | John-Angerson