Biomedical engineers may have found a way of combating one of the deadliest forms of cancer, pancreatic cancer, with a diagnostic method that can catch it, even at its early stages.
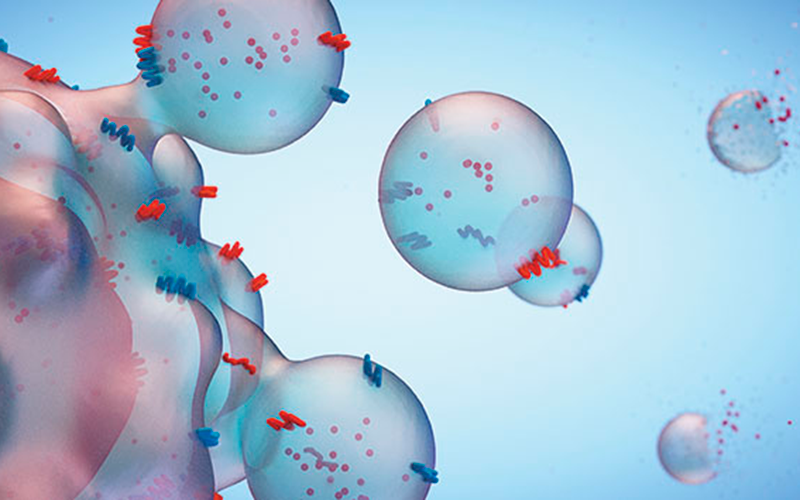
Pancreatic cancer is particularly deadly because it is difficult to detect and diagnose early. Patients usually also have no symptoms until the disease has already spread to other organs, earning it the grim title, “the silent killer”.
In the USA, 74% of patients die within the first year of diagnosis, according to the Hirshberg Foundation for Pancreatic Cancer Research. It’s a bleak outlook.
But biomedical engineering may be able to offer patients hope through
the discovery of a nanoparticle-based technique that could identify pancreatic cancer early in its development.
Extracellular vesicles
Dr Tony Hu, Associate Professor at the Biodesign Institute, Arizona State University, has headed up research devising a fast and inexpensive method that relies on the sensitive detection of extracellular vesicles (EVs) – tiny bubbles of material emitted from most living cells, both normal and tumour.
These EVs are of increasing interest as a resource of diagnostic biomarkers, explains the study, which has been published by Nature Biomedical Engineering.
What led Dr Hu to the closer study of pancreatic cancer was the recognition there is a desperate and urgent need for an early blood biomarker. “Other cancers can be caught at an early stage, but diagnosis for most pancreatic cancer patients remains late stage. Treatment options are also limited. Surgical removal of the tumour is required, but is not possible for most patients diagnosed. We have been working on biomarker discovery and validation for a while. There are currently no effective non-invasive biomarkers for pancreatic cancer diagnosis.”
The only clinically approved blood biomarker for this cancer is the antigen CA19-9, but it is used as a marker for tracking tumour response, not for
cancer diagnosis.
The discovery that EVs can be a good biomarker was a breakthrough and it is in this area the study makes significant further progress.
Dr Hu says: “A circulating tumour cell will secrete EVs and, as a tumour grows and develops, it will secrete more EVs. The beauty of them is their size, ranging from 50 nanometres to 100 nanometres. It means they remain in the blood and are more stable than cancer antigens, for example, so there should be a significant amount present.”
Overcoming problems
But there are critical barriers to their potential being realised. The EV population is huge, since they are derived from a wide variety of tissues. Conventional methods and technology cannot yet readily cope with the challenge of identifying the tumour-derived EVs among the many others.
Isolating them is time-consuming, labour intensive and requires
purification procedures, which are expensive and impractical in a clinical and research setting.
Sample requirements for isolating EVs are also problematic in animal-based research studies, since the blood volume available from mice is limited
and precludes longitudinal studies.
“These were some of the problems we were trying to overcome using our new technology,” Dr Hu says. “We can profile tumour-derived EVs without the isolation step and require only small blood samples, as little as one microlitre. So it is quick and requires minimal preparation.”
Through proteomic analysis, Dr Hu and his colleagues first found that vesicles released by pancreatic cancer tumours carry a surface protein called ephrin type-A receptor 2, or EphA2, that functions as a telltale marker for pancreatic cancer.
The process
The next stage was to test the new method of accurately detecting this protein. Dr Hu explains the key steps: “Small samples of serum or plasma are diluted and applied to a sensor chip coated with antibodies to an EV membrane protein.
EVs bound to the chip by this antibody are then mixed with antibody-coated nanoparticles – one green nanosphere and one red nanorod –that recognise a second EV membrane protein and the pancreatic cancer marker, EphA2.
Only pancreatic cancer-derived EVs bind both nanoparticles, and their close contact on these EVs causes a coupling effect that changes the colour to yellow and markedly increases the intensity of their refracted light, generating a signal that is easily visible
when viewed with a dark-field microscope.”
A series of experiments showed this method identified blood samples from pancreatic cancer with high sensitivity, including those with early stage disease, readily distinguishing them from those of pancreatitis patients and healthy individuals. It detected alterations in EphA2-EV blood levels in pre-
and post-therapy blood samples corresponding to tumour responses to therapy, demonstrating the technique’s power to monitor treatment effectiveness.
Translate into practice
Though this method was patented last year, work is now continuing to evaluate its role in pancreatic cancer diagnoses using a large clinical cohort to validate the findings.
“We would be more confident then to move it forward for approval by the US Food and Drug Administration,” he says.
The research team is also looking at refining the technology so the whole procedure is automated. Such a low-cost, high-throughput format would be more suitable for clinical laboratories.
Significantly, this approach may hold value beyond diagnosis of pancreatic cancer, adds Dr Hu.
“The method can be easily converted to detect other diseases in which EVs may be applied as biomarkers, by changing the antibody target.
“We have research projects looking at lung cancer and tuberculosis.”
Dr Hu has published more than 50 articles in high-impact journals and his research team has received millions of dollars of funding.
“However, the most important moment for me is seeing our technology make a difference to patients and being able to identify cancer patients quickly.”
He adds: “Since this paper was published, I have received many inquiries from patients and their family members. All of them are so encouraging. You can tell how urgently those patients and other people at risk need this tool. We will make the best effort to translate our assay into practice.”
All about Tony
- Joined as Associate Professor at the Biodesign Institute at Arizona State University’s Virginia G Piper Center for Personalized Diagnostics and at ASU’s School of Biological and Health Systems Engineering in 2016.
- Received a PhD from the University of Texas at Austin in 2009, where he focused on developing nanomaterials as biosensors for disease diagnosis.
- Published four nanomedicine-related book chapters, and has given more than 40 seminars and invited presentations at major international scientific conferences.
- Has received five US patents since joining his faculty.