Shahid Nazir Muhammad, a Specialist Biomedical Scientist, considers renal health in transfusion care to inform best practice.
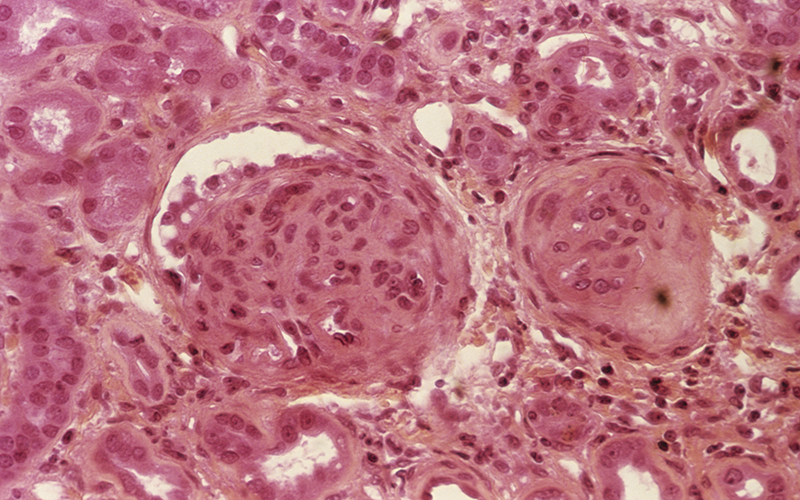
Fig 1 (above) Light micrograph of kidney tissue in a case of glomerulonephritis
Patients with long-term conditions (LTCs) and chronic illnesses (CIs) account for around 50% of GP appointments, 64% of outpatient appointments and 70% of hospital bed days.
Around 70 % of total health and care expenditure in England is attributed to patients with LTCs, who are the most intensive users of health and social care services as their needs are usually more complex than those with single diseases.
Transfusion practices are now incorporating novel pharmacological agents into care, in view of the potential longer term risks and side effects of red blood cell transfusions (RBT). There is ever more need to consider the renal health of patients who require transfusion care, especially as renal function is important in the synthesis of the hormone Erythropoietin (EPO). Where there is renal insufficiency, it can be the difference between morbidity and mortality.
The risks are well reported and have led to a re-evaluation of the criteria for blood product use, but a significant proportion of transfusion practitioners have not modified their approach due to fear of the mortality and morbidity related to anaemia.
Aims
The aims of this work are to highlight the need to consider renal health in transfusion care and research to inform best practice.
Chronic kidney disease
Chronic kidney disease (CKD) can be summated as the steady and consistent reduction in renal function over time. Patients will have no identifiable symptoms and it is largely a “silent”, under-diagnosed disease. Even in the absent of indicators, CKD adds significant burden on cardiovascular health.
It is increasingly being recognised as a global public health problem and a key determinant of poor health outcomes. There is more compelling evidence that disadvantaged communities and backgrounds suffer from marked increases in unrecognised and untreated CKD.
Complex care
There are ongoing concerns about managing anaemia, despite the Better Blood Transfusion initiative from the UK Chief Medical Officers. The initiative began in 1998 and continued until 2012, when it was superseded by Patient Blood Management. The National Blood Transfusion Committee had a major role in overseeing the Better Blood Transfusion initiative in England, where there was a reduction in the morbidity and mortality associated with transfusion documented by SHOT and a reduction of 20% in the use of red cell transfusions.
Large scale trials are still required to see whether EPO has more advantages over RBTs, especially in patients more at risk of transfusion-like reactions.
In one study on the association of EPO use with Hb recovery in anaemic “complex” hospitalised patients, EPO treated anaemic “complex” patients were identified through the combination of a retrospective case review and a systematic reviews. This team established that Hb recovery rate was higher in patients with lower baseline Hb levels, irrespective of EPO use.
LTCs & CIs in numbers
Patients with long-term conditions and chronic illnesses account for around:
50% of GP appointments
64% of outpatient appointments
70% of hopital bed days
Guidelines and frameworks
A practice of 10,000 will have at least 500 patients with stage 3 to 5 CKD, with approximately 15 to 20 of these in stage 4 and five to 10 in stage 5. An elderly and more deprived practice population is likely to have a higher prevalence. About 90% of patients with stage 3 to 5 CKD will have hypertension, 40% will have vascular disease and 30% will have diabetes.
Patients with CKD are roughly 20 times more likely to die from cardiovascular disease than progress to CKD. The all causes mortality rate in CKD is 30 to 60 times higher than in the general population.
Scientists and clinical teams now need to question the clinical implications for transfusing and the leadership and management decisions needed.
Scientists and transfusion practitioners enhancing their skills should review guidelines and frameworks, update skills and understanding relating to strategies for transfusion therapy and should become familiar with NICE definitions of renal anaemia used in CKD and cross-reference with the European Best Practice Guidelines and Kidney Disease Outcomes Quality Initiative.
Clinical factors and the decision to transfuse
Biomedical and laboratory techniques and research have developed over time, especially with respect to blood grouping and cross-matching.
The clinical importance of the red blood cells (RBCs) storage lesion (i.e. the time-dependent metabolic, biochemical, and molecular changes that stored cells undergo) is still lacking.
RBCs can be filtered, washed, frozen, or irradiated for specific indications. RBTs still hold a therapeutic index that exceeds that of pharmacological interventions where RBC replacement is concerned.
Alternatives and indications to RBTs
Reducing the number of inappropriate and borderline transfusions from 80% to 30% reduces patient risk of adverse transfusion outcomes, such as transfusion-associated lung injury and transfusion-associated circulatory overload, as well as transfusion reactions, formation of antibodies. In future, further audit and research into morbidity and mortality prior to and following the guideline introduction would provide key information on patient outcomes. Research to understand and identify suitable alternatives and indications to RBTs for patients with LTCs and CIs has become more important now than it has been in the last decade, and the clinical factors to appreciate renal health need a reputable standing.
Conclusion
Scientists need to be involved in raising awareness and providing education to clinical and medical teams of the intricacy of laboratory practice, but also highlight what treatment alternatives there are that will help preserve renal function over time. Proactive scientists are needed who know the multifaceted nature of CKD. Transfusion practices are being enhanced through service developments and scientists should be at the forefront in decision-making to help inform best practice.
Scientists should not shy away from passing on important knowledge of care that might also have an impact on care pathways. In this regard, if transfusion services are to be effective, scientists need to take ownership to ensure safe and quality-assured practices and engagement at every level, to allow all to voice concerns when required.
Shahid Nazir Muhammad is a Specialist Biomedical Scientist and Co-founder of Renal Patient Support Group.