To mark IBMS History Week, Matt Wilven, IBMS Communications Officer, traces the history of the pregnancy test and looks at the ever broadening market of home testing.
Pregnancy testing can be dated back to an ancient Egyptian papyrus from 1350 BCE. Their medical professionals asked potentially pregnant women to urinate on bags of wheat and barley, claiming that germination of the grain indicated pregnancy: wheat for a boy and barley for a girl. Surprisingly, when researchers tested this hypothesis in 1963 they found that the test for pregnancy was around 70% accurate. Although, it did not account for the sex of the child, the urine of pregnant women (compared to non-pregnant women) did accelerate growth in these grains.
Throughout the middle ages in Europe, pregnancies (and lots of diseases) were often diagnosed by the so-called “piss-prophets”. They claimed to be able to diagnose people on the basis of the colour of their urine (and sometimes the taste). Some were more experimental, mixing wines and alcohols with the urine and observing the results. Again, since alcohol does react to certain proteins in urine, this pseudoscience may have had a moderate success rate.
 The early tests
The early tests

In the 1920s, biomedical science finally caught up with curiosity when a number of laboratories across Europe started reporting that there was a specific hormone – human chorionic gonadotropin (hCG) – which is raised in pregnancy and certain other malignant conditions. In 1927, Selmar Aschheim and Bernhard Zondek introduced a pregnancy test based on the presence of this hormone. “The A-Z test” involved injecting a woman’s urine into an immature rat or mouse and, three days later, analysing its ovaries for an estrous reaction. If, despite its immaturity, the dissected animal had been in heat, the woman was pregnant.
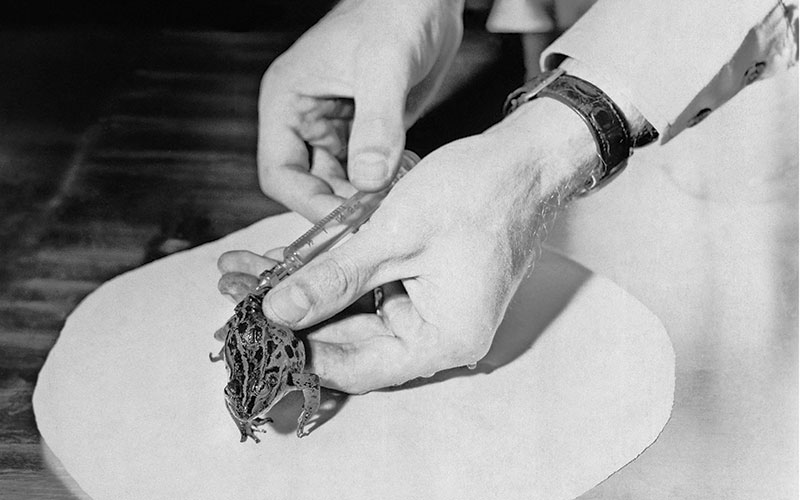
Throughout the 1930s and 1940s, hormone-based research expanded and a number of laboratories developed bioassays to identify hCG – injecting urine into rabbits, frogs, toads and rats. The tests were expensive, involved animal slaughter and took long periods of time to complete. For a while, saying “the rabbit died” was a way of communicating that you were pregnant (it seems that it was not quite clear to people that the rabbit died either way).
By the 1950s, Lancelot Hogben’s discoveries had led to the African toad, Xenopus laevis, being the most used animal for pregnancy testing. They were cheaper than mice, rats and rabbits, the tests were quicker and the animals could be reused. But then, in 1960, Leif Wide and Carl Gemzell developed a haemagglutination inhibition test. This immunoassay used purified hCG mixed with a urine sample and antibodies directed against hCG. The test was much quicker and cheaper than the old bioassays but, at this stage, still relatively insensitive.
Commercially available
In 1966 a radioimmunoassay test for hCG had been developed but the test could not differentiate between hCG and luteinizing hormone (a hormone produced by gonadotropic cells in the anterior pituitary gland which, in females, triggers ovulation and the development of the corpus luteum). This changed in 1972 when Judith Vaitukaitis, Glenn Braunstein and Griff Ross published a paper describing a hCG beta-subunit radioimmunoassay that could specifically measure hCG in the presence of luteinizing hormone - making it useful as an early test for pregnancy.
Until this time, pregnancy testing in the UK could only be performed in pathology laboratories at the request of a medical practitioner. However, after a pregnancy test called Pregnosticon was patented and made commercially available in 1969, high street pharmacists began undertaking haemagglutination inhibition tests at the direct request of the consumer.
In view of this, it was agreed that biomedical scientists could also perform the tests and some set up independent businesses to provide the service.
Home diagnostics
By 1978, a two hour (nine-step) pregnancy test could be bought off the shelf and taken home. It included a vial of purified water, a medicine dropper, a test tube and an assortment of compounds including the red blood cells of sheep. Positive results were 97% accurate and negative results 80% accurate. There was still work to be done but the era of home diagnostics had begun.
The test was up to 99% accurate and gave results in three minutes. This was refined to give results within one minute
In 1988, Unipath launched a lateral flow immunoassay called Clearview (the pregnancy test as we know it today). The urine sample came in through a wick and transferred to a strip, mobilising blue latex particles carrying monoclonal antibodies and moving them towards the part of the strip where the results window was. In a positive sample, hCG in the urine would bind to a line of the antibodies, form a sandwich and trap the blue particles so that they could not go any further – forming a pregnancy indicator. The test was up to 99% accurate and gave results in three minutes.
Within a couple of years, the three minute tests had been refined to give results within one minute. More recently, digital versions have been developed but the scientific principles behind the reaction remain largely the same.
Testing becomes commonplace
Pregnancy tests cemented their place on the shelves of UK pharmacies in the 1970s when the women’s liberation movement embraced the (then complicated) tests because they demystified medicine, empowered women and provided an alternative to the NHS – whose healthcare professionals they often perceived as judgemental and moralistic.
Also, it can’t be ignored that abortion had been made legal in the UK in 1967 and, therefore, the pregnancy test came to prominence in a time when earlier knowledge of pregnancy meant more options for a woman.
“The mainstream success of the pregnancy test was never based on a drive to replace diagnostics but to bring the diagnosis into the home”
Unlike the ultrasound (which came to medical practices in the mid-1950s), these pregnancy tests also had the benefit of not personifying the fetus – which was beneficial for some.
It was not until the 1980s and the advance into lateral flow immunoassay technology that the balance of acceptance tipped for good. Advertisements for the tests could now be found in housekeeping magazines next to baby food and in fashion magazines next to contraception. The relatively unobtrusive and uncomplicated pregnancy test suddenly became a commonplace marker on most women’s pregnancy journeys.
However, there was still a prevailing sense that a pregnancy was not real until it was confirmed by the healthcare services. Even to this day, packaging for pregnancy tests allow for a margin of error and recommend a visit to the doctor.
This inherent referral to healthcare professionals shows that the mainstream success of the pregnancy test was never based on a drive to replace diagnostics but to bring the diagnosis into the home at an earlier stage – allowing a woman to experience the discovery on her own or with her loved ones, rather than with a doctor.
 New launches
New launches

As technology advances, home testing kits become easier and cheaper for medical companies to produce. In the last 10 years, three main types of “direct-to-consumer” medical tests have emerged: blood tests to analyse health markers, DNA “fitness potential” tests and microbiome analyses of the gut.
One of the most successful of the new products is a finger prick blood test which, after being sent off to a laboratory, then provides a report of the geographical history of your DNA – a sort of statistical family tree.
This test is purely commercial and sells on the back of curiosity but, where other types of testing are involved, the transparency of the capital incentive is beginning to raise ethical concerns amongst laboratory professionals.
There was a mixed reception amongst IBMS membership in August last year when news surfaced about HIV self-testing kits being available to buy on the High Street for the first time. Caroline Griffin-Dommersen commented that these tests “should be done in a clinical environment with access to counselling” and Cherie Beckett agreed, saying that the tests could give “low (false) reactives and false negatives in the incubation period”. Other members saw the benefits, citing shorter waiting times and people being too scared to go to a clinic.
Other concerns laboratory professionals have raised about private screening companies include that they may be misleading the “worried well” into non-evidence based testing or screening through manipulative advertising tactics.
Also, that there are potentially large knock-on effects for NHS services when people go to a 10-minute doctor’s appointment with a lengthy report from a private company that they don’t fully understand. Laboratory professionals are already beginning to call for more regulation with regards to what these companies can offer and how they can offer it.
Inaccurate?
An early study in Nature found that up to 40% of the results of home testing kits were inaccurate and the NHS advises that they should not be used as diagnostic tools. Nonetheless, more and more kits are available on the open market and, as the medical profession becomes increasingly focussed on the personalisation of medicine, it is possible that the public will mirror this and become increasingly focussed on discovering their personal medical needs at home.
Yet, despite huge investment in the home testing arena, clever branding and heavily targeted marketing strategies, none of the “direct-to-consumer” medical tests look as though they are about to emerge as commonplace home diagnostic devices. They remain of interest to the few – particularly in the UK where point-of-care testing is free to all. The pregnancy test stands alone in its position as the home testing kit that the majority of people will come into contact with.
The success of the pregnancy test is down to the fact that it is fast, accurate and easy to use, it brings a personal moment into a personal space and it empowers the user by situating them before their options. It has not replaced healthcare services. Rather, it has changed the relationship women have with pregnancy and allowed them to take control of their reproductive healthcare at an earlier stage.
It also answers a fundamental question that we have been asking for thousands of years: “Am I pregnant?”
IBMS History Week takes place on 18 to 24 February. Any members who were involved in pregnancy testing when it occurred in the laboratory, or those who know about the chemistry involved in the new tests, are asked to get in touch by emailing [email protected]
