In 2017, the IBMS awarded research grants totalling almost £25,500 to six Fellows. Here the recipients explain their grant-supported projects.
Dr Avninder S Bhambra
This work looks at modelling of the binding of antitrypanosomal compounds to Trypanosoma brucei PTR1. Neglected tropical diseases (NTD) impose a severe threat to global health through continuous spread and a lack of effective medicines, with more than a billion people affected by these diseases. Sleeping sickness, a two-stage NTD, caused by Trypanosoma parasites, contributes to the burden of NTDs occurring predominantly in eastern and southern Africa.
Treatment for sleeping sickness is dated and potentially lethal, consisting of pentamidine or suramin for the haemolymphatic phase, and eflornithine, melarsoprol or nifurtimox-eflornithine combination therapy for the neurological phase. Advances in antitrypanosomal drug development have been limited and drug resistance is increasing, highlighting the urgent need for a robust pipeline of new drugs to replace existing therapies to support global health strategies.
Work undertaken by Dr Bhambra and colleagues has delivered novel compounds demonstrating significant antitrypanosomal activities against Trypanosoma brucei rhodesiense, while showing limited off-target toxicities. This has provided the platform for the project to exploit in silico drug development approaches to assess potential drug-target interactions and the subsequent design of further compounds with improved on-target and off-target activity profiles.
Helen Lock
Behçet’s disease (BD) is a multisystem inflammatory condition characterised predominantly by urogenital aphthous ulceration and ocular inflammation, the aetiology of which remains to be elucidated. There is no test for BD and diagnosis is based on clinical features. However, it is known that the pathogenesis of BD is complex, involving both the innate and adaptive immune response, causing features of both autoimmune disease and autoinflammatory disease. The lack of clarity in immune pathogenesis means that treatment of BD is targeted at symptom management and prevention of major complications. Some patients do not respond well to initial treatment, which results to prolonged morbidity and impaired quality of life. It is likely that the actions of the many different immune cells involved in Behçet’s pathogenesis are also responsible for a differential response.
In the grant-supported work undertaken by Helen Lock, pre- and post-treatment blood samples will be taken from a clinically defined cohort of patients receiving immunosuppressive or anti-inflammatory treatment, and also from matched controls. Flow cytometry analysis will be used to measure B regulatory (Breg) cell surface markers, a recently identified B-cell phenotype defined as interleukin (IL)-10-secreting inflammatory suppressive cells that may affect treatment response in BD. The presence/absence of different Breg biomarkers will be used to stratify BD patients into groups through post hoc analysis to determine if Breg biomarkers are altered pre- and post-treatment in treatment responders and non-responders. Clinicians will use the grouping to inform treatment and management. The grouped patient will receive personalised treatment, reducing pain and alleviating symptoms.
Dr Olayinka Osuolale
Dengue is the most prevalent arthropod-transmitted virus, with conservative estimates placing half of the world’s population at risk of infection. Transmission of the mosquito-borne dengue virus appears to be largely driven by infections in and around the home, with the majority of cases related to one another – occurring in people who live less than 200 metres apart. Leishmaniasis is responsible for the second-highest number of deaths due to parasitic infection globally and is overwhelmingly associated with poverty. It is almost always fatal, if not treated, and morbidity caused by cutaneous leishmaniasis is also important.
These diseases are neglected, under recognised and under-reported in Nigeria due to lack of awareness by healthcare providers and lack of prioritisation by the public health authorities. Due to poor disease surveillance and lack of reporting, the true incidence and impact of the diseases in Nigeria is unknown.
The research by Dr Osuolale, A preliminary study of a possible dengue fever and Leishmaniasis among university students and staffs in a tertiary institution in Nigeria, aims to investigate cases of febrile infection with possible links to dengue fever and leishmaniasis among the students and staff of Elizade University. The purpose of this study will be to identify epidemiology and immunology of unapparent infection due to dengue disease and leishmaniasis.
Dr Ian Locke
Osteoarthritis (OA) is one of the most widespread skeletal diseases, which negatively affects the quality life of more than eight million people in the UK. It is characterised by cartilage degradation and deterioration of the underlying subchondral bone within the joints, commonly as a result of ageing (long-term wear and tear), joint injury or other risk factors that result in the generation of a pro-inflammatory environment. This environment has been shown to cause suppression and apoptotic death of chondrocytes, the only cell type present in the cartilage matrix, which normally provide cartilage maintenance and repair functions. A decrease in the number of active chondrocytes within the matrix correlates closely with the severity of the cartilage damage.
Although chondrocytes are the only cells present in the cartilage matrix, the picture becomes more complex at the cartilage-bone interface, where development of the pro-inflammatory, pro-apoptotic environment in the cartilage can influence the balance of osteoclast and osteoblast activity, the cells responsible for turnover and maintenance of the bone. Communication between cartilage and bone cells has been demonstrated both in in vivo and ex vivo experiments, and, although the exact nature of this communication has yet to be fully elucidated, this cross-signalling from the damaged cartilage to the bone may contribute to the subchondral bone loss/damage observed in OA.
Dr Locke and his team’s research, Understanding urocortin 1 regulation of chondrocytes and osteoclasts: a new prospective for pharmacological intervention in osteoarthritis, so far suggests that the urocortin (Ucn) system may be a potential candidate for this cross-signalling role, with components of this system expressed in both chondrocytes and subchondral bone cells, and elevated in the synovial fluid of individuals with OA. They have shown that Ucn1 exhibits a dual role as both an essential survival factor for chondrocytes, and a potent inhibitor of osteoclast maturation, motility and resorption. Unlike chondrocytes and osteoclasts, osteoblasts do not express (or respond to) Ucn1, but do express CRF-BP, providing a potential candidate for the regulation of free Ucn1 levels in the local environment.
Understanding the role of the urocortin system in the communication between bone and cartilage cells will provide novel insight into how this system may be manipulated to prevent chondrocyte death and reduce bone resorption – key factors in osteoarthritis and other skeletal disorders such as osteoporosis. It is hoped this will reveal prospects for therapeutic intervention and the development of drugs that mimic the protective function of the urocortin system, to prevent and treat OA and related conditions.
Dr Maria Teresa Esposito
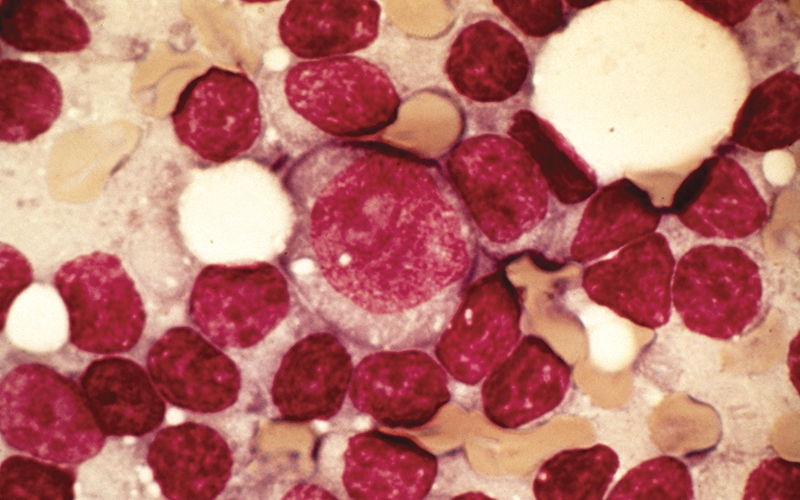
Chromosomal rearrangements of the MLL gene located at 11q23 give rise to aggressive and drug-resistant forms of acute lymphoblastic leukaemia (ALL) and acute myeloid leukaemia (AML), hence the name mixed lineage leukaemia (MLL). No targeted therapeutics are available and the prognosis is dismal, with survival rates of just 20% to 50%.
Although phenotypically MLL can be classified as either lymphoblastic or myeloid, the gene expression profile is unique and distinct from ALL and AML. Transcriptomics-based characterisation and chemical interrogation identified kinases as key mediators in MLL.
Accordingly, inhibitors of kinase GSK-3-β, Flt3, CDK9 and ATM/ATR showed efficacy in MLL animal models; however, their toxicity is still clinically prohibitive. This also implies that efforts to target multiple kinases at the same time might not be clinically feasible.
PP2A is a phosphatase and a critical upstream mediator of the above kinases, found inactivated in solid and haematological malignancies PP2A has been studied extensively in chronic myeloid leukaemia (CML).
Notably, PP2A-activating drugs (PADs) show therapeutic efficacy in AML and CML, with no cytotoxic effect on haematopoietic cells. However, PP2A has not been explored in MLL.
Preliminary data obtain by Dr Esposito’s group show that, like AML and CML, PP2A is inactivated in MLL-AML cell lines. Analysis of MLL-primary AML samples’ transcriptome data, collected as part of The Cancer Genome Atlas (TCGA) project, suggests that epigenetic mechanisms might govern PP2A inactivation in MLL. These data, together with the fast development of PADs, provide a compelling rationale for investigating PP2A as both a prognostic marker and a novel therapeutic target for MLL.
The research grant to Dr Esposito will facilitate the generation of data in support of further collaborative work (Analysis of phosphatase PP2A activity and gene expression in MLL-rearranged leukaemia) aimed at testing the therapeutic strategy of PADs in xenotransplants in in vivo models and extending the study to paediatric patients.
Sarah Maddocks
Chronic wound infections are diagnosed at 100,000 cases per annum and their management is complex, costing the NHS more than £4bn each year. Patients with chronic wound infections are afflicted for months or years and experience persistent or recurrent wound infection that is difficult to resolve. Swabs taken from patients for microbiological assessment frequently recover unusually slow-growing species of bacteria, which grow as very small colonies on agar. Often these bacteria are overlooked as an artefact of culturing techniques and are, therefore, excluded from diagnostic analyses. Designated as “small-colony variants” (SCV), research has suggested that these bacteria are more than a laboratory curiosity and instead could play a significant role in persistent, recurrent infection in wounds.
Supported work by Sarah Maddocks, with Ambikesh Jayal, Small-colony variant bacteria: a laboratory curiosity or cause of persistent, recurrent infection?, proposes to sequence a library of SCVs derived from Pseudomonas aeruginosa, to identify a set of SCV-specific genetic changes that can be developed into a diagnostic tool to detect SCVs in chronic infected wounds. This will be of benefit because SCVs do not grow well in laboratories and produce spurious results with standard diagnostic assays. Identifying patients carrying SCVs using molecular probes would be an accurate and rapid means of diagnosis, allowing clinicians to amend treatments, such as increasing antimicrobial treatment to counter the higher resistance profile of SCVs, and thus limit the likelihood of recurrent infection.
For more information on IBMS grants and awards and how to apply, visit ibms.org/grants-prizes-and-awards
Picture credit | Science Photo Library
