Senior Biomedical Scientist Emma Victory gives practical guidance on how best to make a thick blood film.
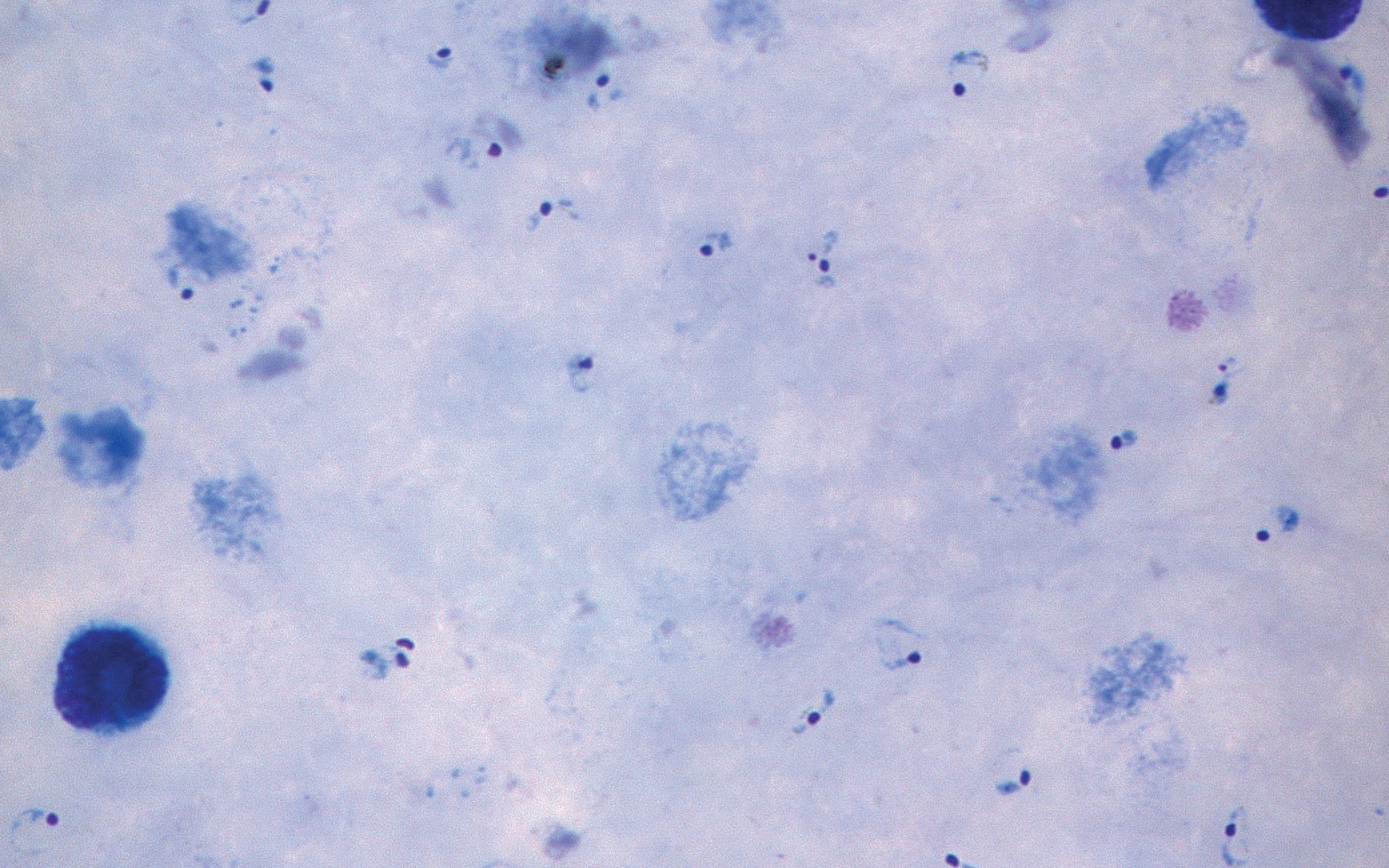
In an increasingly molecular world, microscopy still plays a vital role in malaria diagnosis. Other available methods include rapid antigen tests, quantitative buffy coat, numerous DNA-based assays, as well as clinical diagnosis. But microscopy provides information the other methods cannot. For example, microscopy is the only method which can demonstrate clearance of viable parasites from the blood. Both antigen and DNA-based methods will remain positive for some days (and in some cases weeks) after successful treatment.
In the Public Health England Malaria Reference Laboratory (MRL) we examine thin and thick blood films (where possible) on every patient referred to the lab. Thin films enable species identification of malaria parasites based on morphology of the parasite and changes to the parasitised red blood cells. The parasitaemia (percentage of parasitised RBC) of a patient is estimated using a thin film. This value, which gives an indication of severity of infection, is used to monitor treatment and recovery. Thick films are a concentration technique. In contrast to thin films, a greater volume of blood is used and the entire smear can be examined.
In the hands of an experienced microscopist, thick films are 20 to 30 times more sensitive than thin films for detection of malaria parasites. Relatively speaking, a large volume of blood can be rapidly examined and this is why in some clinical settings thick films are used for screening patients.
Making thick films
We receive many unsuitable thick films at the MRL, possibly because senders are not routinely examining them in their labs or lack experience in doing so. When films are poorly made we may be unable to examine them. If there is a low parasitaemia there may be no detectable parasites on the thin blood film. This may lead to an inconclusive result. Rapid antigen tests are highly sensitive for P. falciparum but they cannot differentiate the non-falciparum species and the sensitivity is much lower for these species. We have molecular assays available in the MRL but they are still not as fast for obtaining a result as a good quality set of blood films in the hands of an experienced microscopist.
Blood films can be made from either a finger prick or from venous blood. They should be made as soon as possible, ideally within two hours of taking blood. Parasite morphology is affected by anticoagulant; the longer the wait between taking blood and making films, the more challenging species identification becomes.
It’s unnecessary to measure the volume of blood used to make thick films (but in practise approximately 5 µl is sufficient). Two or three drops should be placed on the slide and the corner of a slide or an orange stick used to join the drops and spread them into an even layer. It is preferable to make films in the centre of the slide. If too close to the edge, they may be rubbed off in transport, or when placed in a rack to dry.
The shape of the smear is not important – they may be circular or ovoid, or even rectangular. The size should be 1-2cm in diameter. Films should be allowed to dry horizontally on a flat surface to ensure they remain an even thickness. Allow at least 30-60 minutes for thick films to dry before staining or packaging them. Consider the level of humidity in your local environment. In high humidity, thick films will take longer to dry. Films may be dried in a 37 °C incubator for 15 to 60 minutes, although direct heat should be avoided as this may heat-fix the films. It should be just possible to read newsprint through a thick film when it is dry (prior to staining). If this isn’t possible then the film has been made too thick. If too much blood is used, or if the smear is uneven or bumpy, it may not adhere fully to the slide and can flake off before the slide is stained. Or the smear may partly or wholly wash off the slide during the staining process, leaving insufficient material behind to examine.
"If good quality thick films are made and stained correctly they will be much easier to examine"
Different purposes
Thin and thick blood films serve different purposes in malaria diagnosis. Thin films allow visualisation of a monolayer of cells (RBC, WBC, and platelets), along with any intracellular or extracellular parasites. Thin films must be fixed with methanol to preserve all of the details which enable detection and identification of malaria parasites. Thick films are a concentration method. They consist of many layers of RBC stacked on top of each other. Thick films should not be fixed with methanol (or direct heat). During the aqueous staining procedure the unfixed RBC lyse, leaving the remains of WBC and any malaria parasites present behind. If thick films are fixed before staining they will be too dense to examine. When thick films come into contact with methanol vapour unintentionally this can also lead to fixation, e.g. when making thin and thick films if the thins are methanol fixed and then immediately put into a slide box with the thick films this will fix the thicks too, even if only partially, and result in poor or incomplete lysis.
When good quality thick blood films are submitted we have the best opportunity to detect and identify any parasites present in the patient’s blood. This enables us to reach a result more rapidly, consequently promoting more effective patient management.
Thick films are often perceived as too difficult or too time-consuming to bother with, hence they are avoided completely by some laboratories. However, if good quality thick films are made and stained correctly they will be much easier and more pleasant to examine. With a little practice, you might even start to like them as much as thin blood films.
Emma Victory is a Senior Biomedical Scientist at the Public Health England Malaria Reference Laboratory.
